If you have ever experienced those itchy, annoying rashes in the groin area and wondered what’s up? You might be dealing with the tinea cruris symptoms. Yep, that’s the fancy term for what’s commonly known as jock itch. Before you start imagining all sorts of things, let’s break it down and get to know what this is all about.
Tinea cruris is caused by a fungus. Now, I know what you’re thinking. Fungus? Like mushrooms? Well, not exactly. Fungi are a group of microorganisms, and some of them love to live on our skin.
When conditions are just right – warm and moist – these fungi can cause infections. And the groin area, being all tucked away, can provide the perfect home for them.
Now, tinea cruris isn’t the only skin condition caused by fungi. There’s athlete’s foot, ringworm, and a bunch of others. But today, we’re focusing on our main culprit, the jock itch. And if you’re wondering why it’s called that, it’s because athletes, who sweat a lot, are often the ones to get it. But hey, anyone can get it.
Many people develop skin infections during summers. Amongst these, fungal infections of the skin caused by Dermatophytes are common. Dermatophytes belong to a group of fungus that lives superficially on the skin, hair, and nails and causes diseases that are named differently.
| Nails | Onychomycosis/ T. unguium |
| Hair | Tinea capitis |
| Skin | Causes many infections, which are named based on the area of involvement. The common ones include Tinea corporis (body), Tinea cruris (groin), Tinea pedis (foot) |
These fungal infections are generally identified and then treated with some form of anti-fungal medications, usually by a trained healthcare practitioner.
Why is it called Jock itch/ Tinea cruris?
The names of many diseases and medical terms have originated from Latin and Greek languages and cruris in Latin means leg. So, T. cruris essentially means, fungal infection of the inner legs and groin which may also go on to involve buttocks, genitalia and may even extend up to the abdomen.
There is a tendency for increased sweat accumulation in these areas which provides favorable conditions for the fungus to grow.
Fungal infection over the legs and groin can occur if feet and toenails are affected can then spread upwards over the skin when you wear your pants.
What does the infection look like?
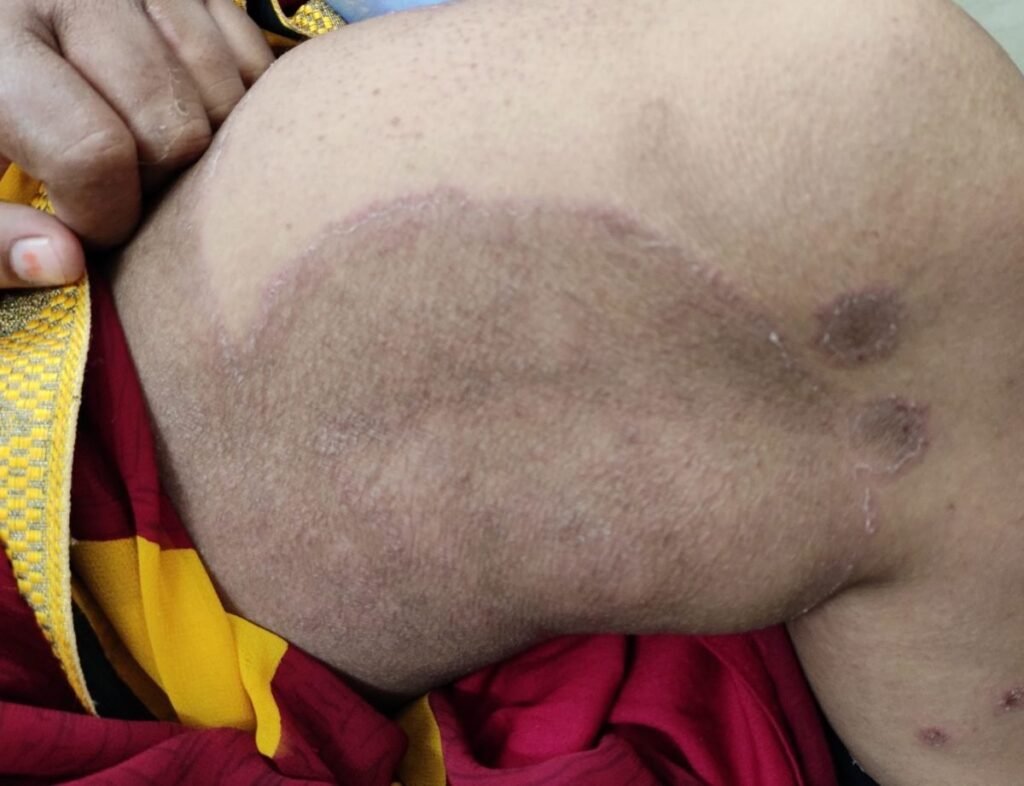
The disease initially appears as a red raised area that is itchy and usually, people go to their doctor when the itching has become so intense that they can’t sleep at night or can’t work without having an urge to scratch.
Your doctor will typically diagnose it just by looking at the rash, which can be seen as a ring-like (annular) lesion with a clear center and red margins.
It slowly keeps on increasing in size as the fungus keeps spreading peripherally or sometimes it may look like an arc or even have irregular borders.
Since the rash looks like a ring it is commonly called “Ringworm” although the infection is not caused by a worm & the label is kind of stuck to the skin condition since the initial cases were identified.
Sometimes, when in doubt, your doctor will take some samples from your skin by scraping it with a slide or a blade and then examine them under a microscope to confirm whether a fungal infection is present or not.
How long will you have to live with Tinea cruris?
Tinea cruris along with other skin infections and especially fungal infections of the nails takes a long time to go away.
Usually, people stop taking the medicines once they see some improvement in the rash. Then they go to their doctor with the complaint that the skin lesions and itching have again become worse, sometimes even more so than they were before starting the treatment. In that case, the treatment will be prolonged or need to be restarted.
- The treatment may need to be taken for about a month or two and sometimes longer in case of nail infection.
- Any decision regarding stopping the medication should be taken after consulting your doctor.
- The medications may have to be either applied to the area of involvement or taken orally or both.
Who is at risk of getting reinfected?
Usually, people who have associated conditions like diabetes, obesity & weak immune system are at increased risk of getting infections and some people are genetically prone to fungal infections in the absence of any of these identifiable factors.
In addition, people who harbor resistant fungal strains can still get reinfected. Over the last few years, dermatologists worldwide have reported an increase in antifungal resistance, particularly with strains resistant to terbinafine (one of the most common antifungal medicines). In these cases, treatment becomes harder, and patients may experience only partial relief or frequent recurrences.
Even if someone clears the visible rash, the fungus can linger in other areas—like toenails, feet, or even on contaminated clothing and bedding. This creates a cycle where the infection re-seeds itself into the groin. If the strain is resistant, standard creams may no longer work effectively, which increases the risk of relapse.
That’s why, when I suspect resistance, I recommend lab testing (fungal culture or PCR) to guide therapy, switching antifungals if necessary, and treating all possible sources—including athlete’s foot and infected nails. Combined with good hygiene, this approach lowers the chances of reinfection, even with resistant strains.
Can Tinea Cruris Be Cured?
Yes—tinea cruris (jock itch) can be completely cured with the right treatment. It is a fungal infection caused by dermatophytes that thrive in warm, moist areas like the groin. With proper antifungal creams, sprays, or oral medications, most people see improvement within 1–3 weeks. In my practice, I’ve seen patients clear up quickly when they stick to the treatment plan and avoid stopping medication early, even if symptoms fade fast.
The challenge, however, is recurrence. Jock itch often comes back if the area isn’t kept clean and dry, or if fungal infections on the feet (athlete’s foot) or nails aren’t treated at the same time. That’s why I tell my patients to wear loose, breathable fabrics, shower after sweating, and avoid sharing towels or clothing.
So yes, it can be cured—but think of it as a two-step process: treat the infection, then prevent it from coming back. Consistency with antifungal therapy and good hygiene practices is what keeps jock itch from becoming a repeat visitor.
How to prevent Tinea cruris symptoms?
It is possible to prevent recurring infections by taking some hygienic precautions like:
- Take regular baths.
- Wash and then dry the body well, especially those areas which tend to sweat a lot.
- Avoid sharing towels or clothes with your friends, spouse, and other family members.
- Changing clothes and especially innerwear every day.
- Avoid wearing tight clothes.
Frequently Asked Questions
Q. Can Tinea Cruris Be Permanetly Cured?
A. Yes, tinea cruris is treatable, especially when caught early. Over the-counter antifungal creams or sprays like clotrimazole or terbinafine usually clear it in 1–3 weeks. However, it has a knack for coming back, especially if you’re prone to sweating, wearing tight clothes, or have other fungal infections like athlete’s foot. The key is not just treatment—but also prevention: keeping the area clean and dry becomes part of your daily routine.
Q. Can Tinea Cruris Spread?
A. Absolutely. It is contagious.
- You can catch it through direct skin-to-skin contact, including during sexual activity.
- It also spreads via contaminated surfaces—like towels, clothes, locker room floors—you name it.
- Funny enough, athlete’s foot and jock itch can pass back and forth on your own body—especially when changing clothes without washing hands or mixing your footwear with undergarments.
Q. Can Tinea Cruris be Sexually Transmitted?
A. So here’s the deal: jock itch itself isn’t classified as an STI, but it can be passed during sex through close skin contact. This means that while it’s not technically an STD, the fungus can spread between partners.